Soap Format Medical Records
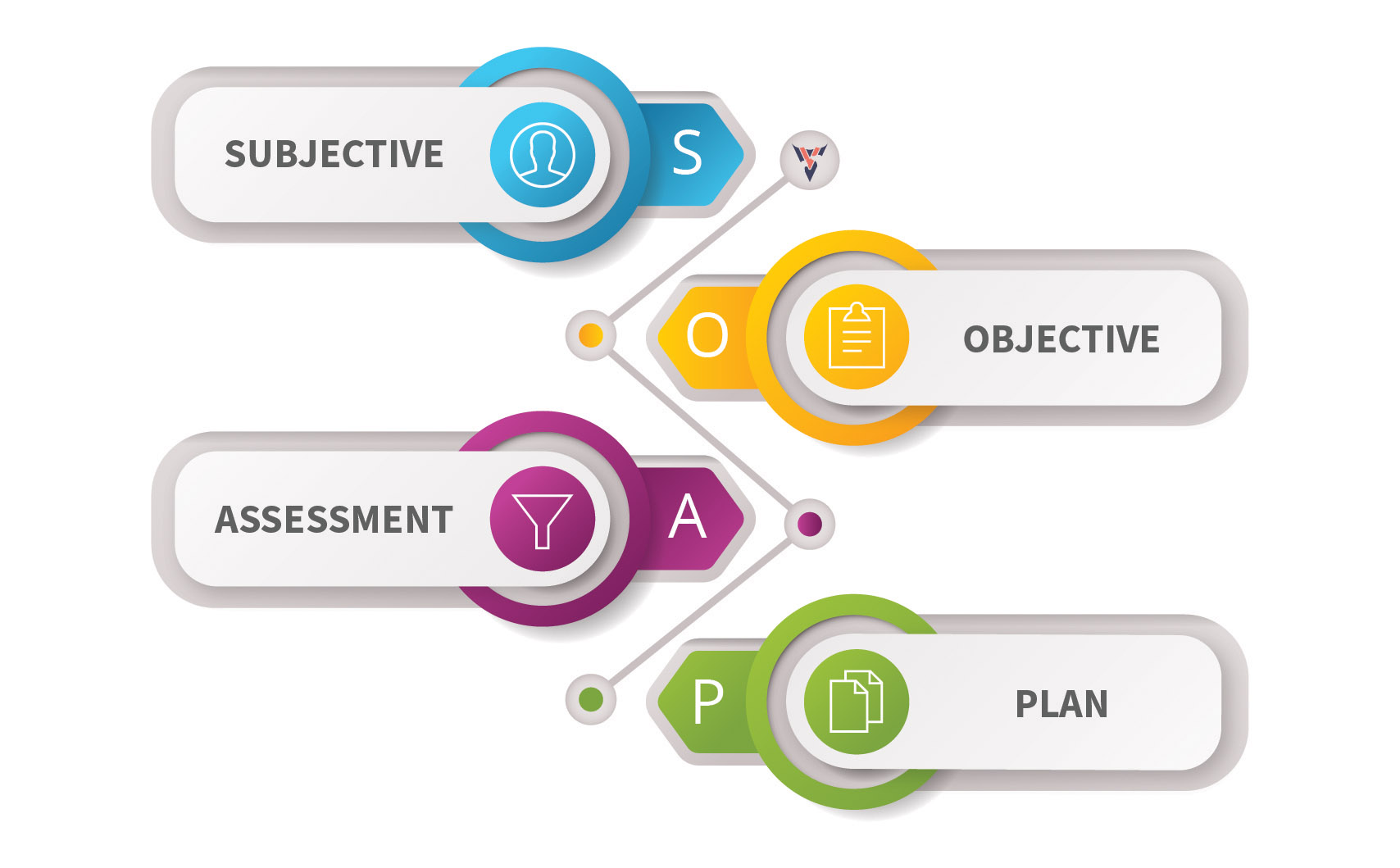
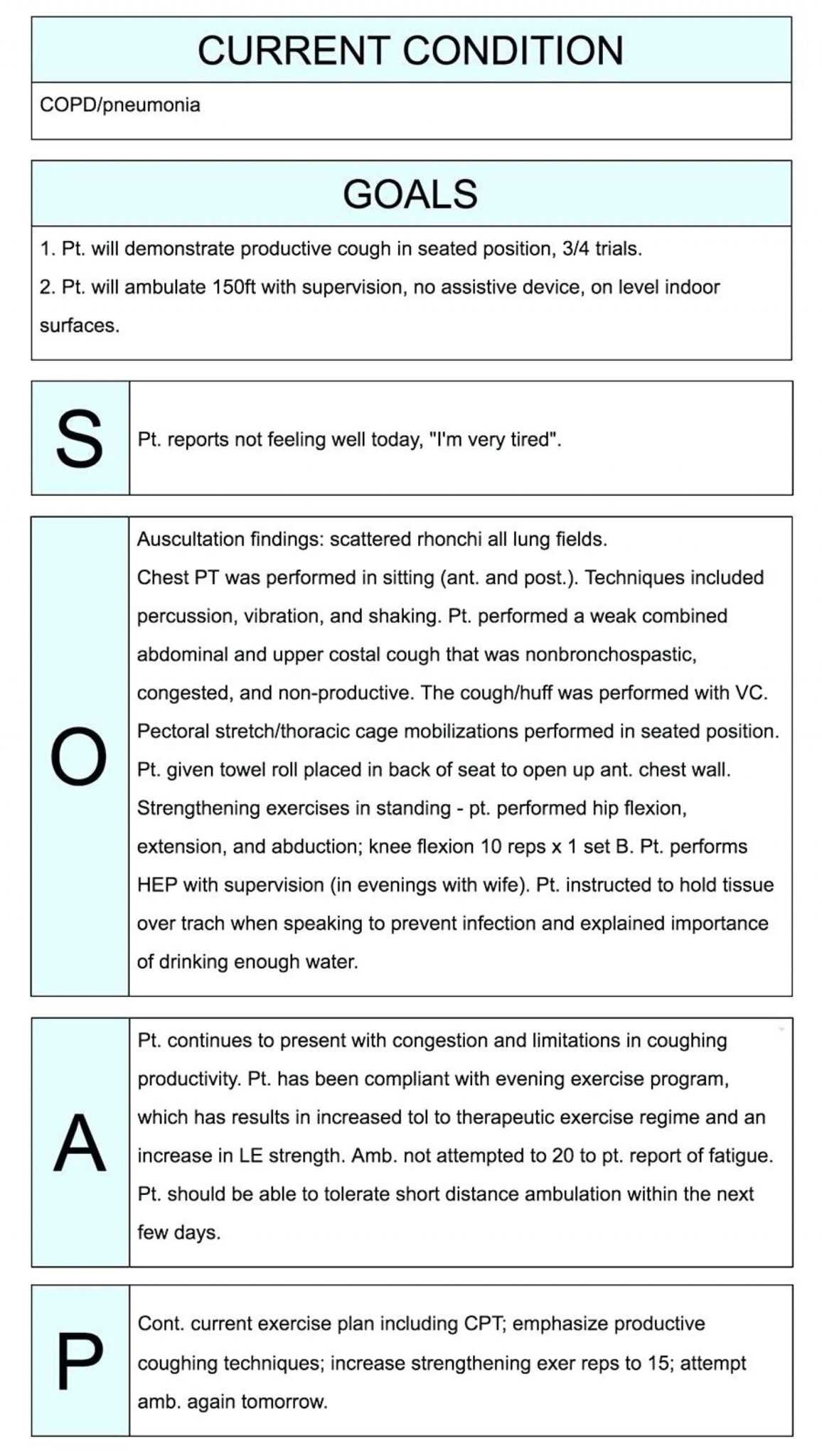
Soap Format Medical Records - Each letter refers to one of four sections in the document. In the soap format, soap stands for subjective, objective, assessment, and plan. Soap notes are a way for healthcare providers to document patient data more efficiently and consistently.
Each letter refers to one of four sections in the document. In the soap format, soap stands for subjective, objective, assessment, and plan. Soap notes are a way for healthcare providers to document patient data more efficiently and consistently.
In the soap format, soap stands for subjective, objective, assessment, and plan. Soap notes are a way for healthcare providers to document patient data more efficiently and consistently. Each letter refers to one of four sections in the document.
Free SOAP Notes Templates for Busy Healthcare Professionals Capterra
Soap notes are a way for healthcare providers to document patient data more efficiently and consistently. Each letter refers to one of four sections in the document. In the soap format, soap stands for subjective, objective, assessment, and plan.
Documenting with SOAP Notes (2 CEs) Premier Continuing Education
Each letter refers to one of four sections in the document. In the soap format, soap stands for subjective, objective, assessment, and plan. Soap notes are a way for healthcare providers to document patient data more efficiently and consistently.
Soap Format In Medical Records Soap Ideas
Each letter refers to one of four sections in the document. In the soap format, soap stands for subjective, objective, assessment, and plan. Soap notes are a way for healthcare providers to document patient data more efficiently and consistently.
35 soap Charting Examples Hamiltonplastering
In the soap format, soap stands for subjective, objective, assessment, and plan. Soap notes are a way for healthcare providers to document patient data more efficiently and consistently. Each letter refers to one of four sections in the document.
Veterinary SOAP notes format of Electronic Health Records (EMRs) 2024
Each letter refers to one of four sections in the document. Soap notes are a way for healthcare providers to document patient data more efficiently and consistently. In the soap format, soap stands for subjective, objective, assessment, and plan.
PPT Medical Records and Documentation PowerPoint Presentation, free
In the soap format, soap stands for subjective, objective, assessment, and plan. Soap notes are a way for healthcare providers to document patient data more efficiently and consistently. Each letter refers to one of four sections in the document.
What’s the Difference SOAP Notes vs DAP Notes Power Diary
In the soap format, soap stands for subjective, objective, assessment, and plan. Each letter refers to one of four sections in the document. Soap notes are a way for healthcare providers to document patient data more efficiently and consistently.
023 Soap Note Example Mental Health Ems Format Template inside Soap
In the soap format, soap stands for subjective, objective, assessment, and plan. Each letter refers to one of four sections in the document. Soap notes are a way for healthcare providers to document patient data more efficiently and consistently.
How to Write Effective Massage Therapy SOAP Notes
Soap notes are a way for healthcare providers to document patient data more efficiently and consistently. In the soap format, soap stands for subjective, objective, assessment, and plan. Each letter refers to one of four sections in the document.
Occupational Therapy Documentation Tips The OT Toolbox Occupational
Soap notes are a way for healthcare providers to document patient data more efficiently and consistently. In the soap format, soap stands for subjective, objective, assessment, and plan. Each letter refers to one of four sections in the document.
Soap Notes Are A Way For Healthcare Providers To Document Patient Data More Efficiently And Consistently.
In the soap format, soap stands for subjective, objective, assessment, and plan. Each letter refers to one of four sections in the document.